
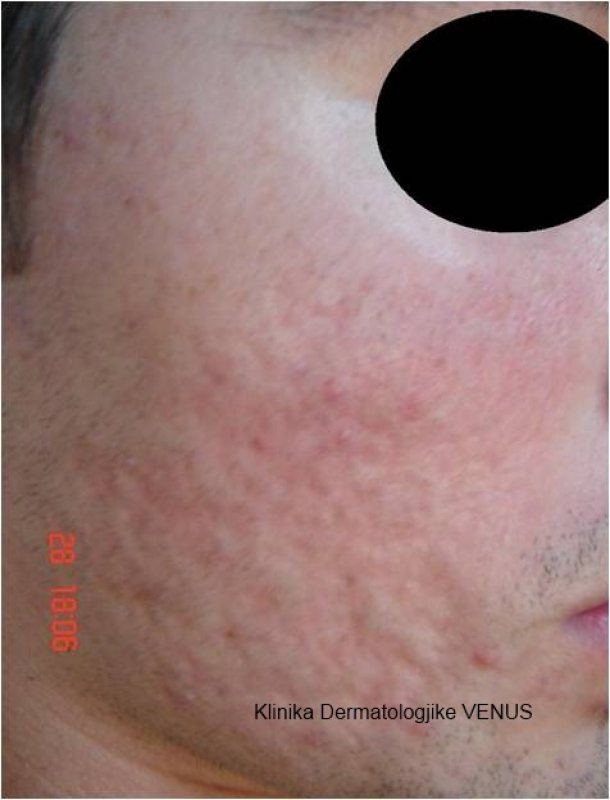
Although it’s common, accurate information about acne can be scarce. This can make it difficult to get clearer skin. The information on this site can help you understand acne and how to successfully treat it.
Myths about acne are as common as the skin problem. One common myth is that you have to let acne run its course.
Dermatologists know that letting acne runs its course is not always the best advice.
Here’s why:
Without treatment, dark spots and permanent scars can appear on the skin as acne clears.
Treating acne often boosts a person’s self-esteem.
Many effective treatments are available.
Not just teens have acne. A growing number of women have acne in their 30s, 40s, 50s, and beyond. Dermatologists are not sure why this is happening. But dermatologists understand that adult acne can be particularly frustrating.
Scars on an individuals skin, no matter how big or small, are often a great cause of concern as they tend to affect confidence. At venus center, our team of world-renowned experts are leaders in the field of laser treatments for the removal of stubborn trauma, surgical, and acne scars, and we’re confident in our ability to bring our patients healthy and radiant skin.
Scars on the skin can happen as a result of numerous factors. Most commonly, patients seek the help of a dermatologist when they are experiencing one of the following:
All three types of scars look very different. An acne scar may come in a number of sizes and depths, with some being called ‘ice-pick’ scars and others being small red pock marks. A surgical scar can form after a patient undergoes surgery and is usually raised slightly above the skin. Scars from trauma can leave discoloration and an uneven texture.
Resurfacing ablative & non ablative
Fraxel Laser Resurfacing is widely known as one of the best laser treatments for the diminishment of body and facial scars. Due to it’s targeted therapy, the laser can be adjusted to treat almost every kind of scar, be it acne, surgical, or trauma related. Laser resurfacing works to penetrate deep within the skin and scar to rejuvenate the appearance by providing a more even skin texture, tone, and color. Though patients may see excellent results after just one treatment, sometimes multiple office visits are necessary depending on the severity of scars present.
This is a common skin disease in children. It is so common that people have given it a few names:
To avoid confusion, we’ll use the medical term atopic dermatitis.
Children often get atopic dermatitis (AD) during their first year of life. If a child gets AD during this time, dry and scaly patches appear on the skin. These patches often appear on the scalp, forehead, and face. These patches are very common on the cheeks.
No matter where it appears, AD is often very itchy. Infants may rub their skin against bedding or carpeting to relieve the itch.
In children of all ages, the itch can be so intense that a child cannot sleep. Scratching can lead to a skin infection.
Because atopic dermatitis can be long lasting, it is important to learn how to take care of the skin. Treatment and good skin care can alleviate much of the discomfort.
Atopic dermatitis (AD) looks different in infants, children, and adults. The following gives you the signs (what you see) and symptoms (what you feel) for each age group.
AD can begin early. A child may be 2 or 3 months old when AD begins. When AD begins early, it often causes:
Parents often worry that their babies are getting AD in the diaper area. A babies rarely gets AD in his or her diaper area. The skin stays too moist for AD.
When AD begins between 2 years of age and puberty, the child often has these signs and symptoms:
Itchy, scaly patches where the rash appeared.
In time, the skin with AD can:
It is rare for adults to get AD. Most people (90%) get AD before age 5. About half (50%) of people who get AD during childhood continue to have milder signs and symptoms of AD as an adult. When an adult has AD, it often looks different from the AD of childhood. For adults, AD often:
Adults who had AD as a child and no longer have AD can have the following:
Extremely dry skin.
Researchers are still studying what causes AD. Through their studies, they have learned that AD:
Runs in families: People who get AD usually have family members who have AD, asthma, or hay fever. This means that genes play a role in causing AD.
Foods do not cause AD. But some studies suggest that food allergies can make AD worse. Children who have AD often have food allergies to these foods — milk and foods that contain milk (e.g., yogurt and cheese), nuts, and shellfish.
Before you stop feeding your child any foods, talk about this with your child’s dermatologist. Children need certain foods to grow and develop normally.
Also called condylomata acuminata
Genital warts are warts that appear in the genital area. There can be 1 wart or a cluster of warts. People get these warts by picking up the human papillomavirus (HPV) from someone who is already infected with this virus.
HPV is a common sexually transmitted infection. It is possible to spread or get these warts even when you cannot see them.
Of the 100 or so types of HPV, just a few can cause genital warts. Some HPV types can cause cervical cancer. Other types can cause anal cancer, cancer of the penis, or mouth and throat cancer. You can get more than one type of HPV.
There are many ways to treat genital warts. Since warts are often stubborn, you may need more than one visit to the dermatologist.
Genital warts appear in various sizes and shapes. Some people get a few warts. Others get many warts. The most common signs (what you see) of these warts are:
Genital warts often have no symptoms (what someone feels). Sometimes the warts itch, burn, hurt, or bleed.
Genital warts can appear on the following areas of the body:
Females
Males
Females and males
Anyone who has sex can get human papillomavirus (HPV), the virus that causes genital warts. At least half of people who have sex have had an HPV infection. It is most common before age 30.
Not everyone who gets an HPV infection gets genital warts. Most people never get these warts because the body’s immune system fights the virus. Most people get rid of the virus in a few years and then are no longer contagious.
People who have a weakened immune system may not be able to fight the virus. When the body cannot fight HPV, genital warts can grow. A person’s immune system can become weak from a disease such as cancer or AIDS. Some medicines, such as those to prevent organ rejection, also weaken the immune system.
Research has found that smokers have a higher risk for getting genital warts than people who do not smoke. It is not clear why.
Sometimes a child gets genital warts. It is rare, but an infected mother can pass the virus to her baby during childbirth. The warts may not show up right away. Genital warts in a child also can be a sign of sexual abuse.
Genital warts spread from a person who has HPV to another person through:
Warts may not appear until weeks or months after sex with an infected person.
People often feel embarrassed by growths in their genital area and do not see a doctor. But seeing a dermatologist can provide peace of mind because you can get a proper diagnosis and treatment.
A dermatologist can diagnose genital warts by examining the warts during an office visit. Sometimes a dermatologist will remove a wart or part of it and send it to a laboratory. This can confirm that a patient has genital warts.
Some genital warts clear without treatment. But removing warts has benefits because treatment:
If you want to treat your genital warts, it is best to see a dermatologist. You should not use a wart medicine that you can buy without a prescription. These medicines treat other types of warts. Genital warts require different treatments.
There are quite a few treatments for genital warts. Before choosing your treatment, a dermatologist will consider many things, including the number of warts, where the warts are, and your overall health.
Treatment may involve a procedure in the dermatologist’s office or a medicine you put on the warts. The following describes the different treatments for genital warts:
Medicine: Often the dermatologist prescribes medicines that you will apply to the genital warts at home. These prescription medicines include:
Procedures: A dermatologist may perform one of these procedures during an office visit:
Sometimes treatment requires more than 1 office visit.
Other treatments: Sometimes medicine is injected into the warts. Interferon, an antiviral medicine, may be injected into genital warts. This treatment is usually used if other treatment fails.
Ask your dermatologist about possible side effects (health problems that can result from the treatment).

Remove Actinic Keratosis and Moles
Actinic keratosis refers to a patch of red, thick, scaly and/or crusty skin lesions that usually range from about 2mm to 6mm or more. These lesions are considered precancerous. Affecting mostly lighter-skinned people, actinic keratosis is caused by overexposure to ultraviolet rays of the sun and tanning beds. Left untreated, up to 10% of lesions will develop into squamous cell carcinoma. More rarely, they will develop into basal cell carcinoma.
CO2 laser treatment can be used to remove actinic keratoses before they become cancerous. It can also remove moles, either for aesthetic or health reasons. Mole treatment is essential for moles that have begun to grow, bleed or otherwise change, as they may be transforming to melanoma – the deadliest form of skin cancer. Any sudden appearance of or change in a lesion, plaque or mole is worrisome and should be brought to the attention of Venus Center dermatologist in order to receive timely CO2 laser mole treatment.
*Disclaimer: Results vary from patient to patient. Results are not guaranteed.
Have you been living with a mark or pigmentation that has always made you feel embarrassed or self-conscious? Freckles, birthmarks, and port wine stains are harmless pigmentations that typically occur at birth, but depending on the shape, size, and location, these marks can detract from one’s appearance or draw unwanted attention. At us our board-certified dermatologists offer a number of treatment options to successfully get rid of dermal and epidermal pigmentations.
To learn more about reducing the appearance of unwanted pigmentation, please do not hesitate to schedule a consultation with the skilled dermatologists at Cosmetic Laser Dermatology. Our team is specially trained to treat a wide range of cosmetic and medical skin concerns, including pigmentation, and can design an appropriate treatment plan for each and every patient’s unique needs.
Birthmarks are benign irregularities on the skin that can appear anywhere on the body. These marks are divided into two groups based on how they are formed.
Vascular (blood vessel) marks develop when blood vessels near the surface of the skin do not form correctly, creating an overgrowth of cells. The most common type of vascular pigmentations include:
Depending on your form of vascular pigmentation and specific skin type, your best treatments may vary. However, the insight of a skilled dermatologist will help you better understand how to treat these conditions for the best looking and longest lasting results possible.
Learn more about abnormal pigmentation at WebMD.com.
There are many types of birthmark and pigmentation treatments available on the market for removing unwanted marks on the skin, but it is crucial to consult with a board-certified dermatologist to avoid any negative side effects or adverse reactions.
At venusderm our patients’ safety is our top priority. We provide only the safest and most advanced laser skin treatments for reducing or getting rid of unwanted pigmentations.
To learn more about our range of laser treatments and their nuanced post-therapy plans, please don’t hesitate to contact us.
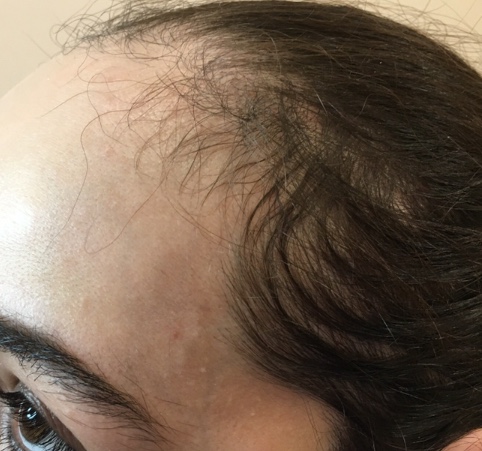
Everyone loses hair. It is normal to lose about 50-100 hairs every day. If you see bald patches or lots of thinning, you may be experiencing hair loss.
There are many causes of hair loss. Women may notice hair loss after giving birth. People under a lot of stress can see noticeable hair loss. Some diseases and medical treatments can cause hair loss.
The most common cause of hair loss is a medical condition called hereditary hair loss. About 80 million men and women in the United States have this type of hair loss. Other names for this type of hair loss are:
Millions of people experience hair loss. Some people see their hair re-grow without doing anything. Others need treatment for their hair to re-grow. Sometimes, hair will not re-grow.
To find out what is possible, you should see a dermatologist. These doctors specialize in treating diseases that affect the skin, hair, and nails.
The reasons for hair loss are many. When hair loss begins suddenly, the cause may be due to illness, diet, medicine, or childbirth. If hair loss is gradual and becomes more noticeable with each passing year, a person may have hereditary hair loss. Certain hair care practices also can cause noticeable hair loss.
Your hairstyle and even some of the products you use on your hair can cause hair loss.
Blow dryers, flat irons, and other devices
Hairpins, clips, and rubber bands
Hairstyles
Improper washing, drying, and combing
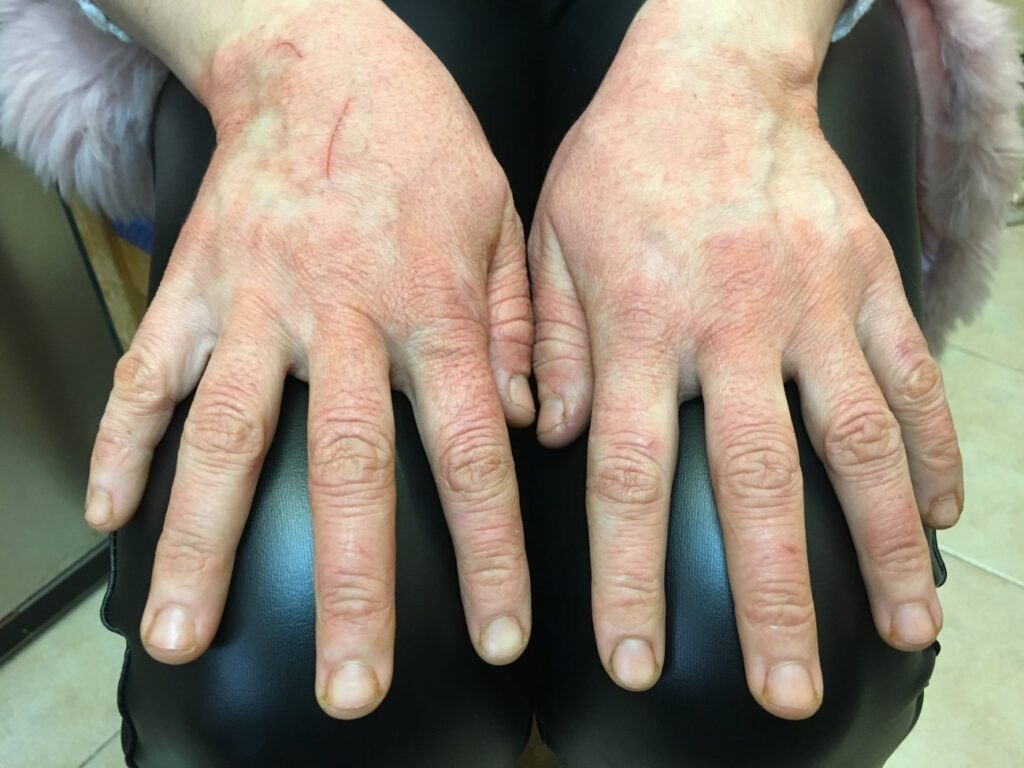
Dry, scaly, and painful hands could be hand eczema
Is the skin on your hands dry, thick, and scaly? Do you have deep, painful cracks on your hands that bleed? You may have more than dry skin. Hand eczema could be the culprit.
Hand eczema can cause the following:
Because it often looks like dry skin, hand eczema can easily be mistaken for dry skin. Unlike dry skin, you need more than a good moisturizer to get rid of hand eczema.
Relief requires finding the cause
Effective treatment begins with finding the cause. Anything that irritates your skin can cause hand eczema. Even something as harmless as water can irritate your skin if your often have wet hands. Many people who frequently have wet hands throughout the day, such as nurses, hair stylists, and plumbers get hand eczema.
Working with chemicals like solvents, detergents, or cement also increases the risk. Hand eczema is common among construction workers and machinists.
Hand eczema can also be caused by an allergic reaction. Some health care workers get hand eczema from wearing latex gloves.
You also have a higher risk of developing hand eczema if you had atopic dermatitis (often called eczema) as a child.
Because so many things can cause hand eczema, finding the cause can be tricky. Until you find the cause and avoid it, hand eczema can worsen.
Treatment includes avoiding the cause
When to see a dermatologist
If you have extremely dry, painful hands and using moisturizer throughout the day fails to bring relief, you may have hand eczema. Without treatment and preventive measures, hand eczema tends to worsen.
A hemangioma is a common vascular birthmark, made of extra blood vessels in the skin. It is a benign (non-cancerous) growth. The exact cause is not known. Hemangiomas are typically not inherited, but others in the family may also have had them.
Treating Hemangioma
The Hemangioma and Vascular Malformations Clinic expertly cares for children with hemangioma.
Request an Appointment
Hemangiomas are more common in girls than in boys. They are more common in premature infants, twins and Caucasian children. Most hemangiomas go through several phases of growth. Then, they start to go away by themselves.
Most appear during the first weeks of life and grow fast for the first 2 to 3 months.
For the next 3 to 4 months, the hemangioma may grow more slowly.
Then, there is usually a period of no change to the hemangioma.
At around 1 year of age, the hemangioma begins to slowly shrink and fade in color. This happens over the next 1 to 10 years. Many go away completely during this time. By the time a child is 5 years old, half of all hemangiomas will be flat and lighter in color. By age 10, many are gone or only faintly visible.
Some hemangiomas leave behind soft, wrinkly skin in areas that were previously stretched out by the hemangioma. Others may leave behind the appearance of superficial (surface) blood vessels. If left over skin changes are noticeable there are procedures that may be used when the child is older to correct the changes. These include surgery and laser treatments.
Types of Hemangiomas
Hemangiomas may occur anywhere on the body. Some children may have more than one. There are three main types:
Superficial (on the surface of the skin): These look flat at first, and then become bright red with a raised, uneven surface.
Deep (under the skin): These appear as a bluish-purple swelling with a smooth surface.
Mixed: These hemangiomas have both superficial and deep components.
Diagnosis
The doctor can usually look at your child’s skin and tell if there is a hemangioma. If the diagnosis is not clear, an ultrasound scan or MRI test may be needed.
The hemangioma may need to be treated if:
The skin “breaks down” and an open sore forms.
It gets infected (especially if it is in the diaper area).
It causes problems with any of the following:
Vision
Breathing
Hearing
Eating
Diaper changes
It is very large or it is a cosmetic concern, such as on the face.
Treatment
Most hemangiomas go away over time without any treatment. If the hemangioma is causing a problem, there are different treatment options.
Your child’s doctor will talk with you about the best choice for your child. This may depend on the size, location and behavior of your child’s hemangioma. Treatments may include:
Topical medicine (on the skin rubbed onto the hemangioma).
Topical beta blockers: These may help lighten the hemangioma and slow its growth. This works best on smaller, superficial hemangiomas.
Topical antibiotic: These are applied when there are open sores with concern for infection.
Oral medicine (taken by mouth). Your child will be watched closely for side effects if taking oral medicine. He or she may need tests before starting.
Propranolol is now the first-line treatment option for concerning hemangiomas. (See Helping Hand HH-V-267, Propranolol forHemangiomas.)
Prednisone is used in select cases that may be resistant to other treatment, or if propranolol cannot be used.
Surgery to remove the growth: This may be considered once the hemangioma has stopped growing or other treatments have failed. Surgery may be used to remove markings left over from hemangiomas.
Laser: This may lighten the appearance of blood vessels left over from hemangiomas.
When to Call the Doctor
Pus
Redness
Pain
Fever over 101 degrees Fahrenheit (taken under the arm)
Skin looks open or oozes
Skin breaks down (ulcerates)
You run out of the prescribed oral medicine.
Your child refuses to take the medicine.
Drowsy
Fussy
Not eating well
Wheezing or having noisy breathing
Feverish and ill while on the oral medicine
If your child is on oral steroids, the medicine must never be stopped suddenly. Be sure to get the prescription filled before your child takes the last dose. The doctor will give you exact instructions on how to slowly stop the medicine when it is time to do so.
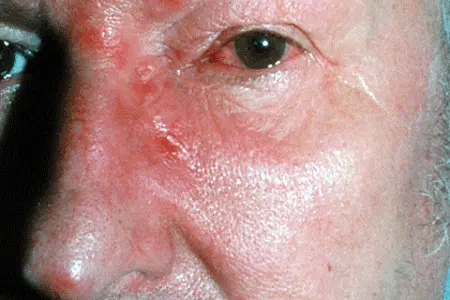
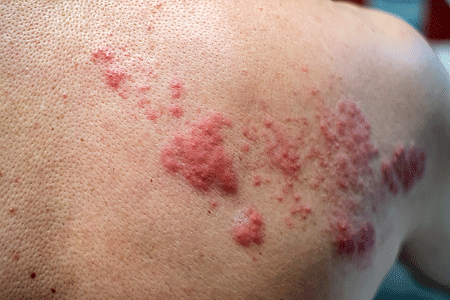
If you have a blistering rash, you want to see a doctor as soon as possible. Should you have shingles, starting prescription medication within 2 to 3 days of developing the rash can dramatically:
If you’ve had the rash for longer than 2 or 3 days, it’s still important to see a doctor. Shingles can lead to other health problems aside from long-lasting pain. For example, when the shingles rash develops on your face, it can affect your eyesight. Treatment can save your eyesight.
A few people who get shingles develop pneumonia, hearing loss, or a disease that causes the brain to swell (encephalitis). It’s important to find signs of these early, so that you can receive treatment.
When you see your doctor, you may hear the medical term “herpes zoster.” This is the medical name for shingles.
Most people who get this disease develop a painful, blistering rash.
Yes, but you cannot give anyone shingles. While you have blisters, you can spread a virus. If that virus infects someone who hasn’t had chickenpox (or the chickenpox vaccine), the person can get chickenpox.
If you had chickenpox, the virus that caused it is still inside your body. When the chickenpox cleared, the virus moved from your skin to your nerves.
Should this virus travel back to your skin, you will get shingles instead of chickenpox.
Hearing the word “herpes” can be confusing. Herpes zoster (also called zoster) is not a sexually transmitted infection (STI). It cannot cause genital herpes. Herpes zoster also doesn’t cause cold sores. Both genital herpes and cold sores are caused by the herpes simplex virus.
The virus that causes shingles and chickenpox is called the varicella-zoster virus. It’s common
Shingles causes a painful, blistering rash on your skin. If you get shingles, you may notice the following:
Although the rash will clear on its own, treatment is important. Taking medication within 3 days of getting the shingles rash can:
Along with a painful, blistering rash, some people can also have one or more of the following:
Fever
Headache
Muscle aches
Stomach pain
Vomiting
These tend to go away as the rash clears.
Some people develop other health problems after the shingles rash clears, which include:
Postherpetic neuralgia (PHN): This is the most common. Occurring where you had the rash, PHN can cause constant tingling, burning, and pain. For others, the pain comes and goes.
Whether the pain is constant or intermittent, it can go on for a long time. You can have PHN for months, years, or the rest of your life. There is no way to know how long it will last.
The pain caused by PHN can become so severe that it interferes with your life, making everyday activities painful. A musician may no longer be able to play an instrument. Some people cannot walk comfortably. It may be difficult to bathe or get dressed. You may have trouble sleeping.
If you have shingles, you can greatly reduce your risk of PHN by getting treated for shingles within 3 days of developing the rash.
Get treated for shingles within 3 days of developing the rash
Taking antiviral medication within 3 days of getting the shingles rash can:
Other health problems that can develop after the shingles rash clears include:
Blindness or loss of some eyesight (if shingles infects your eyes)
Hearing loss
Pneumonia
Encephalitis (swelling of the brain)
Although rare, some people die of shingles.
Treatment can prevent these complications.
An antiviral medication can:
One of three antiviral medications is usually prescribed—acyclovir, famciclovir, or valacyclovir.
To treat your symptoms, dermatologists typically recommend the following:
Pain: Medication that you can buy without a prescription can help, such as:
If you have severe pain, your dermatologist may prescribe a medication that reduces inflammation, such as a corticosteroid.
What is the outcome for someone who has shingles?
Most people get shingles once, but it’s possible to get it again.
If you have a healthy immune system, the blisters tend to clear in 7 to 10 days. The rash tends to go away completely within 2 to 4 weeks. The pain may last longer, but usually stops in 1 or 2 months.
For some people, the pain will last longer than the rash. When it does, it’s called postherpetic neuralgia (PHN), which can come and go or be constant. PHN can last for months, years, or the rest of your life. Treatment can help reduce the amount of pain you feel.
Be sure to tell your doctor if you continue to have pain. Treatment can help you feel more comfortable.

If you have this type of hyperhidrosis, you may sweat:
In one or a few areas of the body: “Focal” means that the excessive sweating (hyperhidrosis) affects one or a few parts of the body. The areas of the body most commonly affected are the underarms, hands and/or feet, and forehead.
On both sides of the body: If the excessive sweating occurs in the underarms, the person usually notices both underarms sweat excessively. The same holds true for the hands and feet.
After waking up: Sweating may begin soon after the person wakes up, but the person usually does not notice damp sheets or wet clothing unless the room is hot.
At least once a week: For many people, it occurs much more often.
If you have this medical condition, you may notice:
Visible sweating: When you are not exerting yourself, do you often see beads of sweat on your skin or have sweat-soaked clothing? Do you sweat when you’re sitting?
Sweating interferes with everyday activities: Does sweating cause difficulty holding a pen, walking, or turning a doorknob? Does sweat drip heavily on to your papers or computer?
Skin turns soft, white, and peels in certain areas: Does your skin stay wet for long periods?
Do you get frequent skin infections on the parts of your body that sweat heavily? Athlete’s foot and jock itch are common skin infections.
Both types cause excessive sweating, but there are some differences.
Primary focal hyperhidrosis
This type of hyperhidrosis usually begins when the person is a child or adolescent. Most people who have this type are otherwise healthy. In medical terminology, the word “primary” means that the cause is not another medical condition.
This type of hyperhidrosis affects one or a few areas of the body, like the underarms.
Man experiencing underarm sweat
In medical terminology, “secondary” means that the excessive sweating (hyperhidrosis) has an underlying cause. The cause could be a:
Medical condition
Side effect of taking a medicine or food supplement
Medical conditions that can cause excessive sweating include:
Diabetes
Frostbite
Gout
Injury, such as head trauma caused by an accident
Menopause
Obesity
Overactive thyroid (hyperthyroidism)
Tumor
The entire body sweats excessively: Sometimes, only parts of the body sweat.
Sweating occurs during sleeping: If you sweat excessively while asleep, it is important to see a dermatologist to learn why this happens.
This type of sweating usually begins when the person is an adult. It also may begin after an accident or frostbite. Many medicines also can cause this type of hyperhidrosis.
Both types of hyperhidrosis can cause people to feel extremely anxious and embarrassed. Students often avoid raising their hand during class. Many teens never date. Adults may hide the sweat stains by wearing layers of clothing or changing frequently throughout the day.
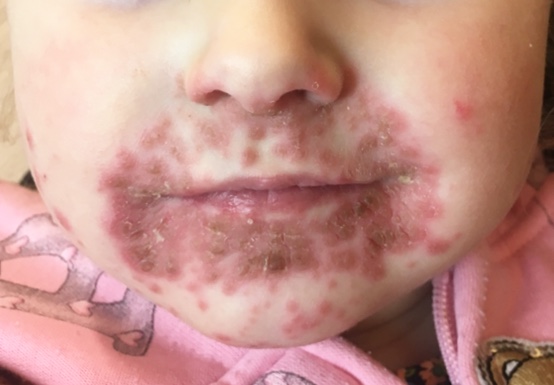
Impetigo (im-peh-tie-go) is a common skin infection, especially in children. It’s also highly contagious.
Most people get impetigo through skin-to-skin contact with someone who has it. Children and athletes like wrestlers and football players often get it this way.
It’s also possible to get it by using something infected with the bacteria that cause impetigo. You can get it from an infected towel or sports equipment. Wearing infected clothing is another way to get impetigo.
Staph and strep cause most cases of impetigo. These bacteria cause impetigo by getting into the body. They can get in through a cut, scratch that barely breaks the skin, or bug bite. A rash, sore, or burn also provides a great entry point for the bacteria.
A child may get impetigo by scratching itchy eczema or chickenpox. The scratching breaks the skin, making it easy for the bacteria to get inside.
Sometimes impetigo develops on unbroken skin.
While highly contagious, impetigo is rarely serious. It often clears on its own in a few weeks.
Treatment, however, is recommended. By treating it, you reduce your risk of developing complications. Without treatment, the infection can cause new sores or blisters to develop for several weeks. The infection can also go deeper into the skin. This can be serious.
Treatment also reduces your risk of spreading impetigo to others.
This is the most common type. It goes through these stages:
The infection can spread to other areas of the body, where you’ll see this process begin all over again. This is one reason treatment is so important.
This type causes fluid-filled blisters, but without redness on the surrounding skin. When a person has bullous impetigo, you’ll see it progress as follows:
Children aged 2 to 5 years old are most likely to get this extremely contagious skin infection.
Anyone, however, can get impetigo. Older children and adults get it. Adults often catch impetigo from an infected child.
Some athletes have a higher risk of catching it. Because of the skin-to-skin contact in sports like wrestling and football, these athletes often get impetigo. The bacteria that cause impetigo thrive in warm, humid places, so swimmers also have an increased risk.
Summer can catch it from touching an infected surface or sharing a towel with a swimmer who has impetigo.
People who live in hot, humid areas get more cases of impetigo. In the United States, people often catch it in the summer or fall.
Bacteria cause this highly contagious skin infection.
Most people develop it when the bacteria, usually staph or strep, invade injured skin. A scrape on your skin is often enough to get infected. The bacteria may also get in through a cut, insect bite, or anything else that damages the skin. Once inside, the bacteria cause an infection in the top layers of the skin.
Sometimes, the bacteria invade uninjured skin and cause impetigo.
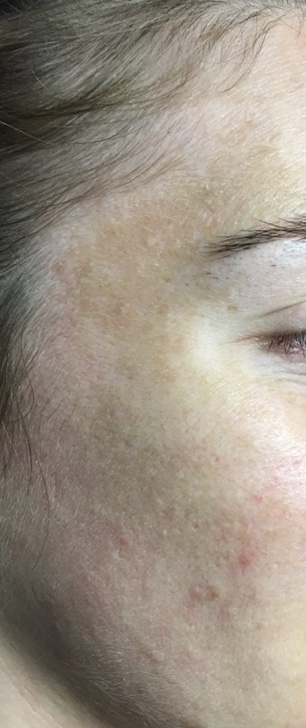
The spots and discoloration usually develop on the face, particularly on the chin, nose, cheeks, and forehead. People with melasma typically notice darkened brown or gray patches on their skin. Melasma can also develop on other parts of the body that receive frequent sun exposure, like the neck, arms, and hands. Because the condition is especially common among pregnant women, it is also referred to as the pregnancy mask.
Prolonged sun exposure can also increase the risk of developing facial patches and other forms of skin cancer. The dermatologists at Venus Center suggest scheduling an appointment at the first sign of new growths or spots and discolorations of the skin. Read more about facial hyperpigmentation at WebMD.com.
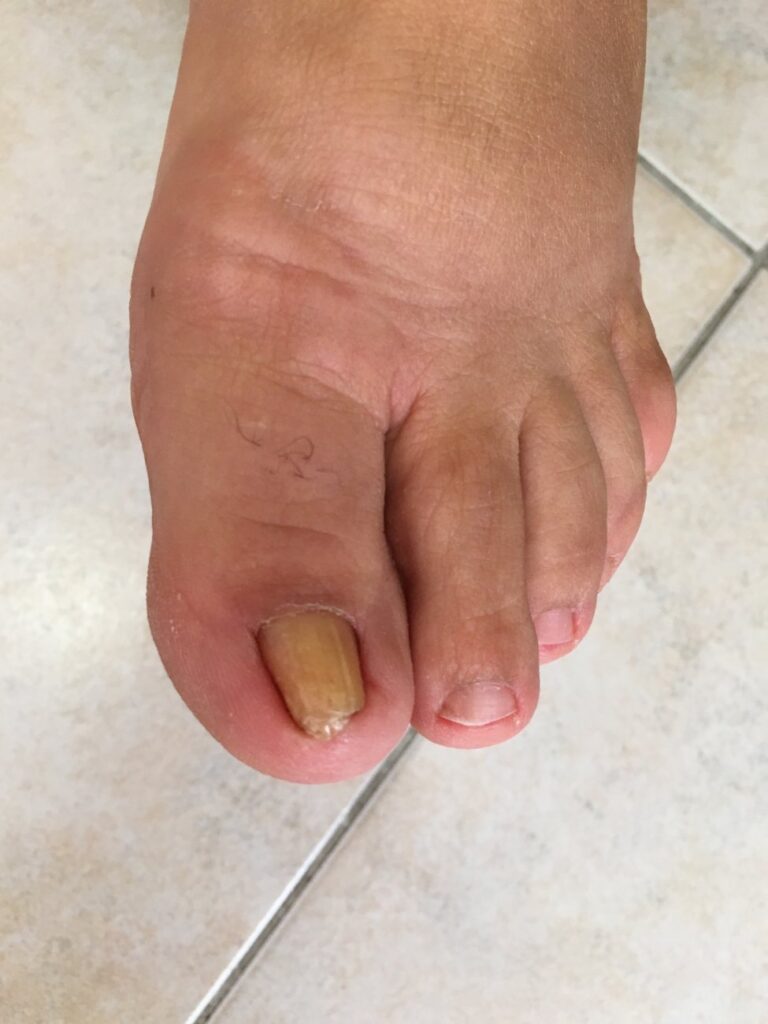
Ingrown nails. It happends when nails grow in the nailbed. Healthy nails grow straightforward. But sometimes, the edge of the nail gets in your skin. It is usually diagnosed in the thumb. To make sure it does not happen follow these steps:
If the problem is persistant, consult a dermatologist.
Moles are common. Almost every adult has a few of them. Adults who have light skin often have more moles. They may have 10 to 40 moles on their skin. This is normal.
Most moles appear on the skin during childhood and adolescence. Moles will grow as the child (or teen) grows. Some moles will darken, and others will lighten. These changes are expected and seldom a sign of melanoma, the most-serious skin cancer.
For adults, new moles and changes to existing moles can be a sign of melanoma. Caught early, melanoma is highly treatable.
Here are 3 facts that can help you find melanoma early and get treatment:
There are also times when a dermatologist should examine a child’s mole. You’ll find pictures and descriptions of moles on a child’s skin that should be examined at:
A mole on your body usually has these traits. It’s:
The most-serious skin cancer differs from moles in that it tends to show one or more of the following traits:
A = Asymmetry. One half is unlike the other.
B = Border. An irregular, scalloped, or poorly defined border.
C = Color. Is varied from one area to another; has shades of tan, brown, or black; is sometimes white, red, or blue.
D = Diameter. Melanoma are usually greater than 6mm (the size of a pencil eraser) when diagnosed, but they can be smaller.
E = Evolving. A mole or skin lesion that looks different from the rest or is changing in size, shape, or color.
If you see a mole or new spot on your skin that has any of the ABCDEs of melanoma, immediately make an appointment to see a dermatologist.
Dermatopathology is a subspecialty of dermatology that studies skin disease at a microscopic level. It encompasses both the diagnosis of individual patients through the examination of skin biopsies, and the study of the causes of skin diseases at the cellular level. Dermatopathologists work in close association with dermatologists. In fact, many doctors train in both specialties.
Dermatopathology is a consultative service to the referring physician and not simply a laboratory test. An accurate microscopic interpretation of the biopsy is important in the selection of appropriate therapies. All cases processed in our laboratory are examined by a board-certified dermatopathologist.
One of the greatest challenges of dermatopathology is the high number of different skin diseases. There are an estimated 1500 different rashes and skin tumors, including variants. Therefore, dermatology and dermatopathology are among the most complex specialties in medicine, and we are proud to offer you both through our practice.
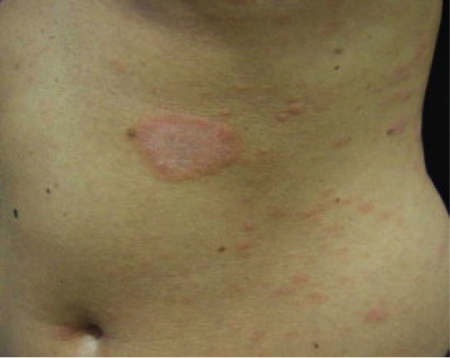
Pityriasis rosea: This common skin disease causes patches on the skin. Your dermatologist may call the large patch a mother patch. The smaller patches are daughter patches.
Pityriasis rosea (pit-uh-rahy-uh-sis row-zee-ah) is a common skin disease that causes a rash. This rash usually disappears on its own without treatment. You can expect to see the rash for about 6 to 8 weeks. Sometimes the rash lasts much longer.
Some people who develop this rash see a dermatologist to get treatment for the itch.
When people get pityriasis rosea, they often have the following signs (what you can see) and symptoms (what you feel):
Mother patch: The first sign of this rash is a single patch on the skin. Called a “herald” or “mother” patch, this patch is the only patch on the skin for about 2 weeks. This patch can get large. It feels scaly. People who have fair to olive-colored skin will see a pink or rose-colored patch. In people who have dark skin, the color varies from violet to dark gray.
Daughter patches: Within a week or two, more patches appear on the skin. These patches are smaller and may appear on the chest, abdomen, back, arms, and legs. Sometimes these patches develop on the neck, face, and elsewhere on the skin. Patches can even develop inside the mouth. These patches are oval shaped. If many patches appear, these new patches may form a pattern on the back. The pattern often looks like a Christmas tree.
Patch-free zones: Patches rarely appear on the face, scalp, palms, or soles.
Itch: The skin can itch. About half (50%) of the people have itchy skin. The itch tends to worsen when the skin gets warm, such as when a person works out or takes a hot shower.Sometimes, a mother patch does not develop, just lots of daughter patches. Some people may get only a mother patch. It is rare for a person to get only daughter patches or a mother patch.
Who gets pityriasis rosea?
People of all ages and skin colors get pityriasis rosea, but this skin disease is more likely to occur:
Between 10 and 35 years of age.
During pregnancy.
No one knows what causes pityriasis rosea. Research shows that it is not an allergy. We also know that fungi (plural of fungus) and bacteria do not cause this skin disease. A virus may be the cause, but researchers have yet to prove this.
It is possible that a virus causes pityriasis rosea, but this skin disease does not seem to be contagious. It does not seem to spread from one person to another.
Pityriasis rosea usually goes away without treatment. You can expect to have the rash about 6 to 8 weeks before it disappears. Some people have it for 2 weeks. Occasionally, it lasts longer than 8 weeks.
If a patient has unbearable itching, a dermatologist may prescribe a medicine to help relieve the itch. Sometimes a dermatologist prescribes light treatments for the itch.
Pearly penile papules (PPP), technically called hirsuties papillaris genitalis, are not sexually transmitted. Their cause is unknown, although they are more common in men in their twenties and thirties, and are also more common in uncircumcised males.
PPP affects many men and can be an embarrassing condition.
Pearly Penile Papules (PPP), are small, dome-shaped bumps that can appear on the sulcus or around the corona of the penis. These bumps, or papules, may be skin-colored or slightly lighter than the skin. It is believed that nearly 1 out of 5 men will be affected with PPP in their lifetime. Though some men choose to leave this condition untreated, many men find their appearance to be embarrassing, causing social and emotional affects. Luckily, treatment for PPP is simple and effective.
Some men choose to leave this condition untreated, as the papules are generally asymptomatic. However, many men find this condition to be embarrassing in intimate situations and suffer detrimental social and emotional effects from leaving them untreated. Treatment for pearly penile papules is typically quite simple and effective through carbon dioxide laser treatment by a qualified dermatologist.
The most effective, painless, and safest treatment for the successful removal of Pearly Penile Papules is performed with the latest generation CO2 laser. This CO2 laser provides optimal results because of its unique ability to specifically target particular areas without damaging nearby tissue in any way. Before the treatment begins, a numbing cream will be applied to the affected area. Once the cream has fully activated,is been applied laser co2
Psoriasis (sore-EYE-ah-sis) can appear anywhere on the skin. When it forms on the scalp, it is often called scalp psoriasis.
Scalp psoriasis can extend beyond the scalp. It can appear on the forehead as shown in the picture on this page. Sometimes, it extends to the back of the neck or appears behind the ears.
On the scalp, psoriasis may need different treatment. The skin on the scalp is thicker. Hair can get in the way.
Psoriasis can appear anywhere on the scalp. Sometimes a small patch develops, which can be easy to hide with hair. Scalp psoriasis also can cover the entire scalp. When psoriasis appears on the scalp, you may notice:
Scalp psoriasis causes many people discomfort. Some people feel embarrassed. Treatment can ease these problems. There are many safe and effective treatments. Some people get relief from a medicated shampoo or solution. A few of these can be purchased without a prescription.
But scalp psoriasis can be stubborn. Many people see a dermatologist for treatment. A dermatologist can tell you what can help. The following types of treatment can help scalp psoriasis:
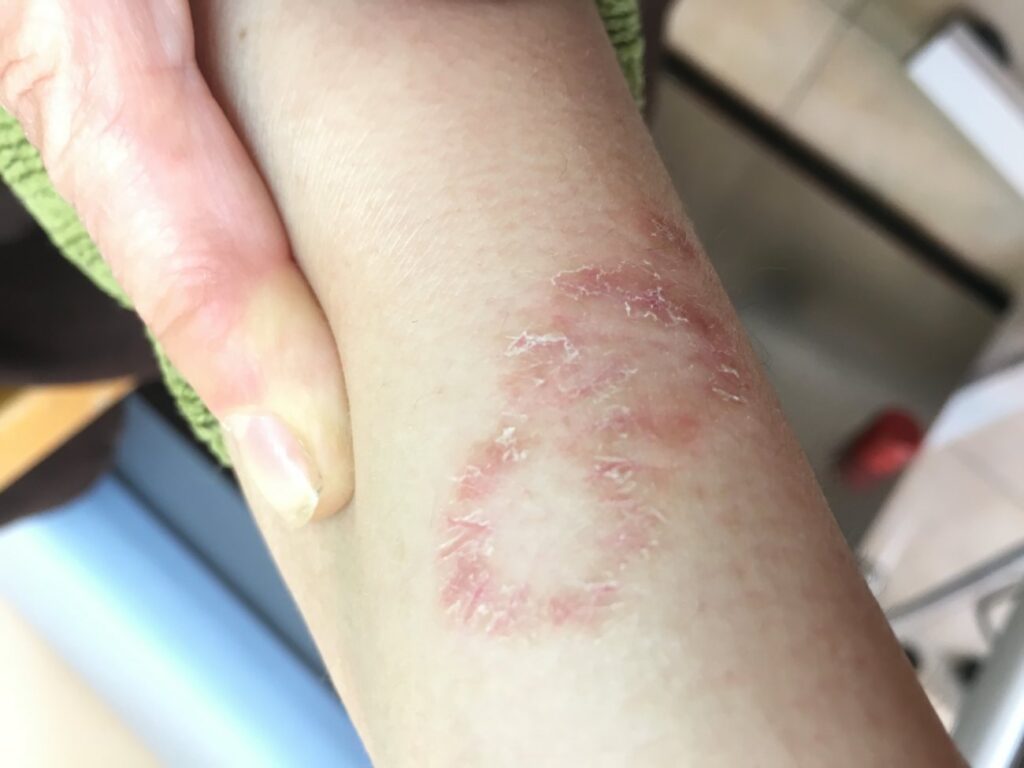
If you have ringworm, you may think you have worms in your skin or a disease caused by worms. You have neither. Ringworm is actually a skin infection caused by fungus. No worms involved.
The name “ringworm” probably comes from the rash that many people see. On the skin, the rash often has a ring-shaped pattern and a raised, scaly border that snakes its way around the edge like a worm.
Ringworm is common. You’ve already had it if you had:
Ringworm can appear on just about any part of your body. On the palms, soles, scalp, groin, and nails, the rash lacks the ring-shaped pattern. On the soles and groin, ringworm also has a different name.
No matter where ringworm appears on the body, treatment is important. Without treatment, the rash tends to grow slowly and cover a larger area. You can also infect other areas of your body.
Treatment can get rid of the ringworm and stop the itch, which can be intense. Because ringworm is contagious, treatment can also prevent you from spreading it to others.
Ringworm is an infection caused by fungus. You can get ringworm anywhere on your skin.
On most areas of the skin, it causes ring-shaped patches. What you see, however, changes when ringworm grows on the feet (bottoms and sides), palms, nails, groin, beard area, or scalp.
If you notice any of these signs or symptoms, you should see a dermatologist. You could have ringworm or another type of skin infection. Treatment can cure a skin infection.
Rosacea (rose-AY-sha) is a common skin disease. It often begins with a tendency to blush or flush more easily than other people.
The redness can slowly spread beyond the nose and cheeks to the forehead and chin. Even the ears, chest, and back can be red all the time.
Rosacea can cause more than redness. There are so many signs and symptoms that rosacea has four subtypes:
If you are living with rosacea, you are in good company. Some famous people have struggled with rosacea:
Because rosacea has so many signs and symptoms, scientists created 4 subtypes of rosacea. Some people have more than one rosacea subtype at the same time. Each subtype requires different treatment.
Signs and symptoms
Signs and symptoms
Signs and symptoms
his subtype is rare. When it does occur, the person often has signs and symptoms of another subtype of rosacea first. The signs of this subtype are:
Rosacea can affect more than the skin and eyes. Because rosacea is a chronic (long-lasting) skin disease, it can reduce a person’s quality of life. Many people report problems at work, in their marriage, and with meeting new people. Surveys and studies report that living with rosacea can cause:
Anxiety and depression
To give you the best results, treatment often begins with a bit of education. While medicine or laser treatment can help reduce or clear signs of rosacea, your everyday habits may cause a new flare-up.
Learning how to do the following can help reduce flare-ups:
Think sun protection 24/7
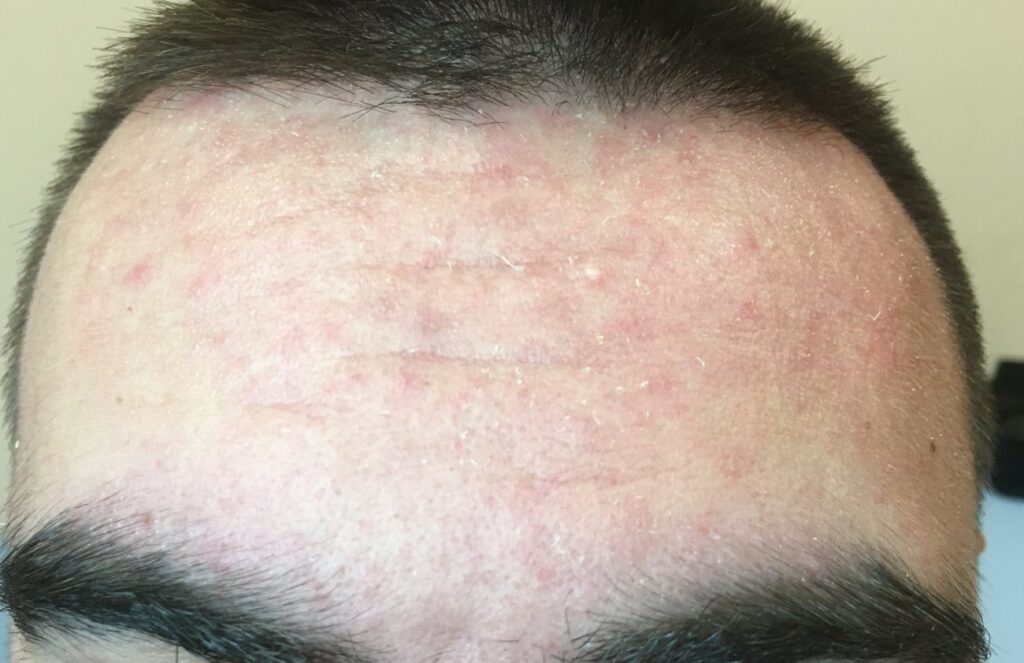
This is a very common skin disease that causes a rash. When this rash appears, it often looks like the one pictured above. The skin tends to have a:
Many infants get cradle cap. This is a type of seborrheic dermatitis (seb-uh-ree-ick dur-muh-tahy-tis) that develops in babies. Scaly, greasy patches form on the baby’s scalp. The patches can become thick and crusty, but cradle cap is harmless. Cradle cap usually goes away on its own within a few months.
Babies also get seborrheic dermatitis in their diaper area and elsewhere. In the diaper area, the red rash often is mistaken for diaper rash. A few babies get seborrheic dermatitis that covers much of the body with red, scaly patches.
No matter where the seborrheic dermatitis forms, it tends to permanently disappear between 6 months and 1 year of age.
Seborrheic dermatitis causes:
In adults and adolescents, the skin can:
Patches form where the skin is oily:
Patches form where the skin is oily, such as on the scalp, face, and in the ear canals.
When an infant gets seborrheic dermatitis, it tends to form on the scalp and is known as cradle cap. Signs and symptoms of cradle cap include:
In infants, seborrheic dermatitis also can form on the face, usually on a baby’s eyelids, around the nose, or ears. It also forms in the diaper area. In a few babies, seborrheic dermatitis covers most of the body.
Most infants seem unbothered by seborrheic dermatitis. Cradle cap sometimes itches.
Researchers are still studying what causes this common skin disease. From what they have learned, it appears that the cause is complex. Many factors seem to work together to cause seborrheic dermatitis. These factors may include the yeast that normally lives on our skin, our genes, living in a cold and dry climate, stress, and a person’s overall health.
By studying seborrheic dermatitis, researchers have learned the following:
If you are taking any of the following medicines, your risk for seborrheic dermatitis increases:
Infants (scalp): Called cradle cap, this tends to completely disappear without treatment. If treatment is necessary, a dermatologist may recommend:
Infants (skin beyond the scalp): This, too, will clear. If treatment is needed, a dermatologist may prescribe a medicine that can be applied to the child’s skin.
Adolescents and adults (scalp and rest of body): After infancy, seborrheic dermatitis usually does not go away without treatment. For the best results, a dermatologist will consider many factors before creating a treatment plan. Treatment may include:
Adolescent or adult: A few people see seborrheic dermatitis clear without treatment. More often, seborrheic dermatitis lasts for years. It tends to clear and flare without warning. Treatment often is necessary to control it.
Also called solar keratosis
An AK forms when the skin is badly damaged by ultraviolet (UV) rays from the sun or indoor tanning. Most people get more than one AK. When you have more than one AK, you have actinic keratoses, or AKs.
Anyone who has many AKs should be under a dermatologist’s care. Most people who have many AKs continue to get new AKs for life. AKs are considered precancerous. Left untreated, AKs may turn into a type of skin cancer called squamous cell carcinoma.
By seeing a dermatologist for checkups, the AKs can be treated before they become skin cancer. If skin cancer does develop, it can be caught early when treatment often cures skin cancer.
Actinic keratosis refers to a patch of red, thick, scaly and/or crusty skin lesions that usually range from about 2mm to 6mm or more. These lesions are considered precancerous. Affecting mostly lighter-skinned people, actinic keratosis is caused by overexposure to ultraviolet rays of the sun and tanning beds. Left untreated, up to 10% of lesions will develop into squamous cell carcinoma. More rarely, they will develop into basal cell carcinoma.
CO2 laser treatment can be used to remove actinic keratoses before they become cancerous. It can also remove moles, either for aesthetic or health reasons. Mole treatment is essential for moles that have begun to grow, bleed or otherwise change, as they may be transforming to melanoma – the deadliest form of skin cancer. Any sudden appearance of or change in a lesion, plaque or mole is worrisome and should be brought to the attention of Venus Center dermatologist in order to receive timely CO2 laser mole treatment.
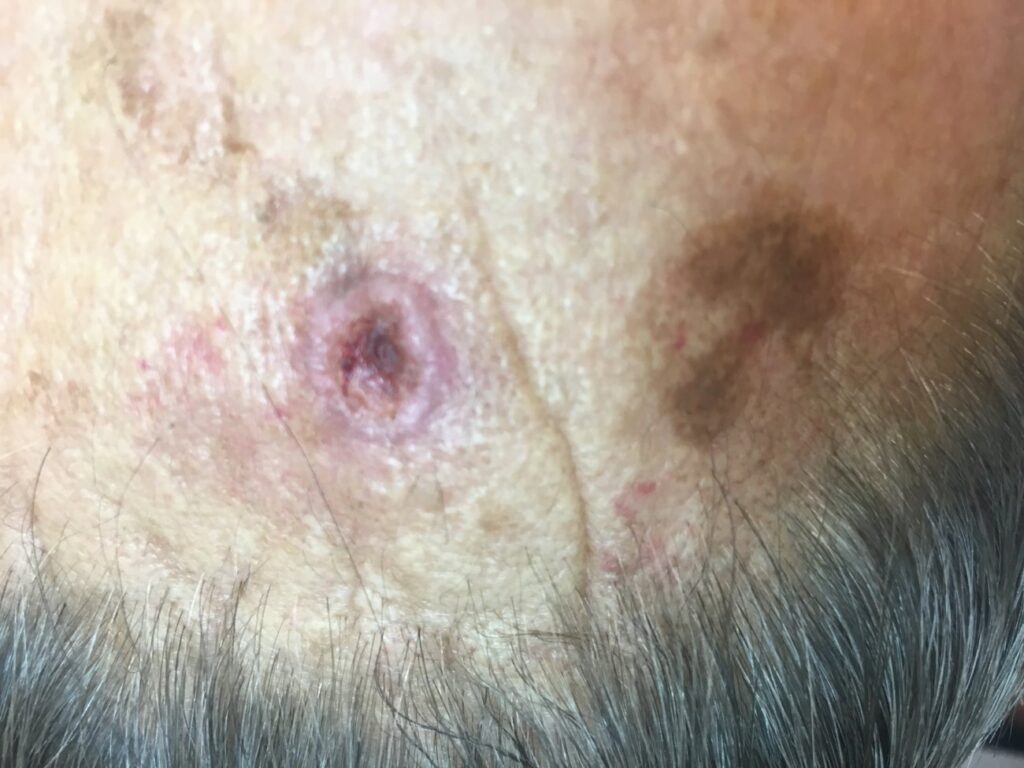
Skin cancer results from an accumulation of damage from the sun’s ultraviolet (UV) radiation. Additional factors that can contribute to the disease include a compromised immune system or exposure to harmful substances such as toxins or radiation.
Other risks include:
Skin cancer develops due to a mutation of skin cell DNA in the epidermis or the top layer of the skin.
There are three major types to be aware of:
*Disclaimer: Results vary from patient to patient. Results are not guaranteed.
This develops in the squamous cells just under the surface of the skin, particularly in areas commonly exposed to the sun, such as the face, arms, hands, legs or ears. SCC is distinguished by a flat, crusted lesion or a scaly, firm reddish skin nodule that may bleed.
The deadliest type, it forms in cells called melanocytes, which are found in the bottom layer of the epidermis. A melanoma is different from the other two cancers because it usually forms in areas that don’t see the sun. It manifests as a multi-colored black, blue, red, tan and/or brown spot, a mole that bleeds, a change in color or an abnormally-shaped lesion.
There is also a precancerous lesion called actinic keratosis (AK), which is a rough, scaly, reddish lesion that develops on the face, arms, or anywhere exposed to a lot of sunshine. While AK is not life-threatening, the lesion may turn cancerous over time if left untreated.
The National Cancer Institute states that 20 percent of Americans and over 59% who live in the Southern USA—regardless of skin color, skin type, ethnicity, or race—will have skin cancer at some point. For those with symptoms, a skin cancer screening by a medical professional at our Skin Cancer Center can detect the disease early enough for an easy successful treatment.
In fact, a screening is useful for those lacking symptoms yet, due to risk factors such as frequent sun exposure, are at a higher risk of skin cancer.
Once skin cancer has been diagnosed, various types of treatments are available, but which treatment is chosen depends on both cancer type and the patient’s overall health.
Common treatment options include the following:
Mohs surgery – A precise procedure known as Mohs micrographic surgery has been in practice for decades and remains the most common treatment method because the cure rate is very high.
Excision – The targeted growth is removed with a sharp surgical razor in one of two ways: excisional biopsy (full removal) and shave excision (a less invasive method for removal of superficial lesions).
Cryotherapy – Super-cooled liquid nitrogen, between -346° F and -320° F, is used to destroy diseased cells without damaging the adjacent tissue.
Electrodesiccation with curettage – An older treatment that is particularly effective for small squamous cell carcinoma or basal cell carcinoma on the chest or back. In this procedure, a curette is used to scrape off cancerous tissue. Then the wound is closed with the superheating properties of electrodescication.
Topical medications – Effective topical treatments include 5-fluorouracil (5-FU), an at-home treatment that destroys superficial cancerous cells, and Imiquimod (IMQ), a new type of medication that triggers the immune system into destroying the malignant tissue. Picato™ can also be used for superficial skin cancer treatment as well as photodynamic therapy (see below).Actinic Keratosis And Photodynamic Therapy
Actinic keratosis is a pre-cancerous skin lesion resulting from direct sun exposure. It commonly appears on the face, ears, back of the hands, and other sun-kissed areas of the body. It resembles an age spot but is scaly, reddish and feels rough to the touch. In fact, it is often felt before it is seen. It commonly starts out pink before darkening into a reddish-brown.
Actinic keratosis, left untreated, increases the risk of skin cancer.
Mohs Surgery: Precision Cancer Treatment
Everyday Preventative Measures
Follow these common, practical tips for skin cancer prevention in San Diego:
Skin cancer is preventable and highly treatable, especially when diagnosed early. Learn more by contacting us
Dermatologist examines mole on patient’s neck
While sheltering in place during the coronavirus pandemic, people are tackling all sorts of DIY projects from baking bread to sewing COVID-19 masks. Some people are even trying DIY surgeries, such as removing a mole or skin tag.
Dermatologists caution that at-home surgery can go seriously wrong quickly and unexpectedly. Trying to remove a mole or skin tag at home could cause a deep-seated infection. You could cause unstoppable blood loss. To get life-saving care, you’d have to go to the emergency room (ER).
If you have a mole or skin tag that you want to remove, you can still contact a dermatologist.
During the coronavirus pandemic, some dermatologists offer telemedicine appointments. This allows you to consult with a dermatologist while sheltering in place. If the spot on your skin needs immediate care, you can schedule an in-person visit.
Whether the spot on your skin requires immediate medical care or can be removed later, you want to see a dermatologist. Here are five reasons why:
A mole that grows, itches, or changes in any way could be skin cancer.
If you remove this mole at home, the cancer can spread before it’s found.
Find and treat skin cancer. Skin cancer can appear on your skin in many ways. It can look like a changing mole, new growth, or scar. When you see a dermatologist, you receive the care you need to find out whether or not you have skin cancer. If you have skin cancer, you can receive expert medical care.
If you remove a mole at home that’s actually a skin cancer, you can leave behind microscopic cancer cells. These cancer cells can multiply and spread deep into the tissue beneath your skin. If you have melanoma, these skin cancer cells can spread quickly throughout the body. This is why melanoma is called the deadliest skin cancer.
Caught early and treated, melanoma is highly treatable.
Control infection risk. When doctors cut into skin, they follow guidelines that dramatically reduce the risk of infection. Without this knowledge, you risk developing a serious infection, which can require a trip to the ER.
Minimize scarring. Any time you wound your skin, you risk developing a scar. Dermatologists have the expertise required to reduce scarring.
Prevent loss of movement due to scarring. If you cause a scar on skin that covers a joint, such as a knuckle or elbow, the scar can limit how far you can move your finger or elbow. Dermatologists understand this risk and use their expertise to help avoid this.
Avoid difficult-to-stop blood loss. Before treating you, your dermatologist will ask questions about your medical conditions and medications that you take. This information helps your dermatologist know what could cause difficult-to-stop bleeding and take necessary precautions.
Dermatologists also have the in-depth medical expertise required to remove skin growths with the least amount of injury. Without this knowledge, it’s easy for you to nick a blood vessel or cut into a vein unexpectedly.
It’s understandable that you may want to do everything you can to treat yourself at home during the coronavirus pandemic. Dermatologists are helping people do this when possible. They’re also providing information to help you avoid unnecessary risks, such as DIY mole removal.
Telangiectasias are small blood vessels that you can see just below the surface of the skin. They may appear as a single vessel or a cluster of vessels. Telangiectasias can also appear in the mouth, eyes, and brain.
Small blood vessels become stuck in a wide open position. This makes them more visible. It is not always clear why this happens. Some may have related conditions, such as rosacea
This problem is more common in women and people who are 40 years of age and older. The risk may also be higher in people who have other family members with this problem.
Symptoms are red lines under the skin that:
May appear in a lacy pattern
Can appear anywhere on the body, but are most common on the face, nose, and legs
Are often painless
May have a burning feeling
May bleed
Diagnosis
You will be asked about your symptoms and health history. A physical exam will be done. This is often enough to make the diagnosis.
Treatment is not always needed. This problem rarely causes health concerns. However, some may not like how they look.
Make-up can be used to cover the red patches. The blood vessels may also be destroyed with laser therapy or chemicals. These treatments are not right for everyone.
There are no known methods to prevent this health problem.

The PHAROS EX-308 Excimer is a monochromatic, xenon-chlorine laser. It is a small handheld device that emits ultraviolet light at a wavelength of 308nm (nanometers), a wavelength found to be more focused on treating various types of skin conditions without damaging the surrounding, untargeted areas.
If you’re one of the 7 million-plus Americans who suffers from vitiligo or one of the 8 million+ who suffer from psoriasis, you know all too well that theseskin conditions can greatly affect your appearance, which in turn, can be a blow to your self-esteem.
Vitiligo is the development of depigmented skin due to loss of melanocytes, the cells that give skin its color. The result is patches of skin that are significantly lighter than your normal skin color.
Psoriasis, on the other hand, is a chronic autoimmune condition that changes the texture of your skin in various parts of your body. The result is thick, flaky skin that becomes inflamed and itchy.
Chronic sun exposure can damage the skin’s pigment and produce white spots, a condition known as idiopathic guttate hypomelanosis (IGH). This is most common on the arms and legs.
Some people develop permanent white scars after surgery or treatment with liquid nitrogen.
These skin ailments do not have a known cure. Vitiligo and psoriasis both can only be managed, usually by topical or oral medications or, in some cases, light therapy can be effective, as well. IGH and white scars have no other effective treatment other than with the Excimer laser
However, a better, safer way of managing both vitiligo and psoriasis could be the Excimer laser.
Because the Excimer emits a specific wavelength of UV light (308 nm), this helps improve skin more effectively. Other UV-B laser systems have a range of wavelengths (290-320 nm) that don’t address skin that has lost pigmentation or has become rougher in texture as effectively because the laser energy is less focused and precise. This means longer laser treatment sessions and more sessions to get results.
The Excimer laser, with its focused doses of controlled UVB light. It is similar to traditional light therapy but with a big difference – the specific activation means that your treatments are shorter (usually less than half an hour) and that fewer sessions are required to get the results you want.
For vitiligo, the Excimer helps you regain normal pigmentation quicker, while for psoriasis, you get clearer skin faster and more effectively. If you have dark skin, the Excimer is particularly effective in reducing the prominence of vitiligo. If you suffer from psoriasis, the laser can more effectively address hard-to-reach or more persistent areas, including:
The Excimer is non-thermal (doesn’t use high heat) and non-ablative (doesn’t burn), which means it is virtually painless, though results vary due to patient skin sensitivity. The finger-switch on the proprietary handpiece delivers treatment to stubborn, hard-to-reach places, all while protecting healthy, unaffected skin.
Additionally, the small handheld device makes treatment a snap at the Cosmetic Laser Dermatology office; there is no need for a lengthy office visit. Your hectic schedule is practically undisturbed.
Yes. Because of the targeted laser, the surrounding skin or tissue remains untouched and unharmed. Your risk of premature skin aging is reduced.
Your skin does not thin, bruise, suffer stretch marks, or experience other side effects that other treatments such as steroids or oral medications can render.
Eight (8) sessions are typical (compared to 25 or more with conventional light therapies), although your treatment plan may vary.
Each plan is customized by a CLDerm dermatologist based on the following:
Treatment is virtually pain-free. During and after treatment, you may experience slight warmth on the skin, but this is normally mild and temporary – anesthesia is unnecessary.
Afterwards, you could experience 3-4 days of redness, itchiness, and mild irritation, but other side effects are uncommon.
Vitiligo (vit-uh-lie-go) causes the skin to lose its natural color. Patches of lighter skin appear. Some people develop a few patches. Others lose much more skin color.
Vitiligo can also affect other parts of your body. A section of hair can turn white. Some people lose color inside their mouths. Even an eye can lose some of its color.
What causes this color loss is still a mystery. We do know that vitiligo is not contagious. It is not life-threatening.
But vitiligo can be life-altering. Some people develop low self-esteem. They may no longer want to hang out with friends. They can develop serious depression. Most people have vitiligo for life, so it’s important to develop coping strategies.
But vitiligo is more than a “cosmetic problem.” It is a medical condition. People get vitiligo when their body attacks its own melanocytes (meh-lan-oh-cites) — the cells that give our skin, hair, and other areas of the body color.
These cells live in the skin, hair, lips, mouth (inside of), nostrils, genitals, rectum, eyes, and inner ear. When the body attacks them, the result can be a few light-colored patches on the skin. Others see widespread loss of skin color. Hair can develop a white streak. This can happen to hair anywhere on the body, including the top of the head, an eyebrow, or eyelash. If the body attacks these cells in the inner ear, the person may develop hearing loss.
What causes the body to attack these cells is not entirely understood. Vitiligo may be an autoimmune disease. These diseases happen when the person’s immune system mistakenly attacks some part of the body.
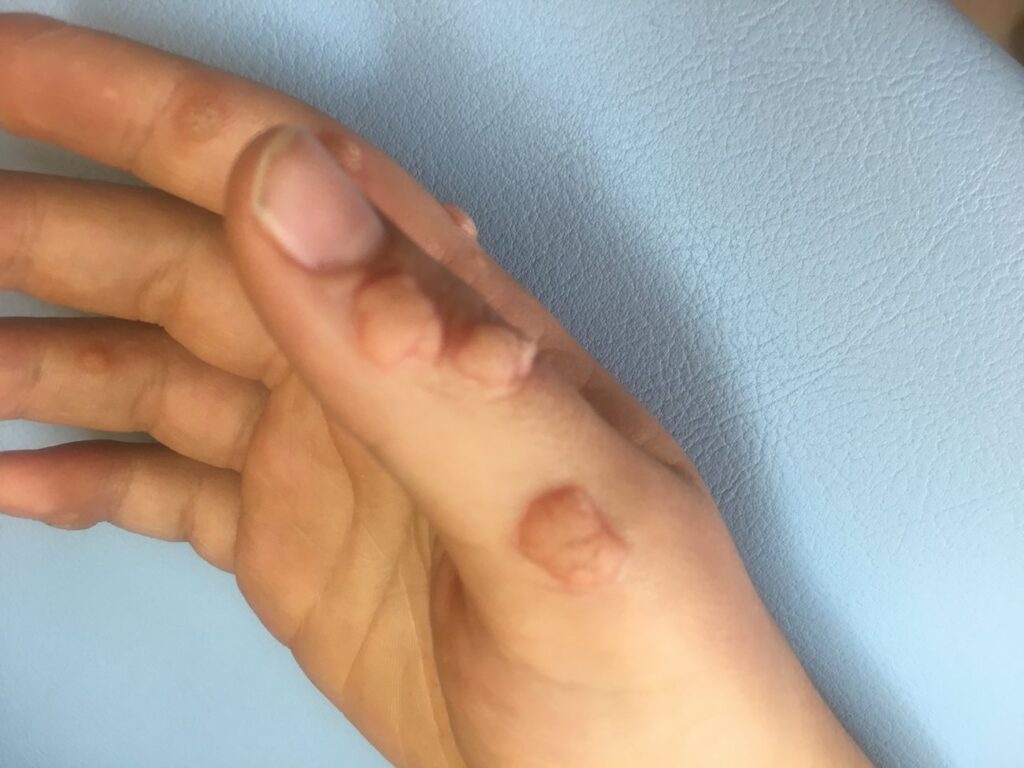
Warts are benign (not cancerous) skin growths that appear when a virus infects the top layer of the skin. Viruses that cause warts are called human papillomavirus (HPV). You are more likely to get one of these viruses if you cut or damage your skin in some way.
Wart viruses are contagious. Warts can spread by contact with the wart or something that touched the wart.
Warts are often skin-colored and feel rough, but they can be dark (brown or gray-black), flat, and smooth.
Common warts have these traits:
Plantar warts have these traits:
Flat warts have these traits:
Filiform warts have these traits:
HIV weakens the immune system, so the body often cannot fight the virus that causes the warts.
Anyone can get warts. Some people are more prone to getting a wart virus (HPV) than others. These people are:
In children, warts often go away without treatment. A dermatologist should treat warts that hurt, bother the child, or quickly multiply.
Viruses called human papillomavirus (HPV) cause warts. It is easier to catch a virus that causes warts when you have a cut or scrape on your skin. This explains why so many children get warts. Warts also are more common on parts of the body that people shave such as the beard area in men and the legs in women. You can spread warts from one place on your body to another.
Warts can spread from person to person. You can get warts from touching a wart on someone’s body. Some people get a wart after touching something that another person’s wart touched, such as a towel. It often takes a few months for warts to grow large enough to see.
Xanthelasma are yellow growths on or near the eyelids. They can be flat or slightly raised. They form when deposits of cholesterol (lipid or fat) build up under the skin. While xanthelasma themselves are not harmful, they can be a sign of heart disease.
Some think xanthelasma is linked to having high cholesterol levels (fat in blood) passed down from parents. This is because up to half of those with xanthelasma have high cholesterol. But the other half have normal cholesterol. So, some think other causes such as inflammation lead to xanthelasma.
Anyone can get xanthelasma. But you are more likely to get it if you:
Xanthelasma is also more common in women and those of Asian or Mediterranean descent.
A doctor can tell if you have xanthelasma by looking at the skin around your eyes. They may order a test to check the levels of lipids in your blood. This can show if there is a potential health issue causing your xanthelasma.
Xanthelasma do not go away on their own. They tend to stay the same size or grow larger. While they are generally harmless, you may want to remove them for cosmetic reasons. Xanthelasma is treated by removing the deposit with:
Most treatments are successful in removing xanthelasma. But there are potential side effects like:
Also, xanthelasma can return after surgery.
Take steps to manage your cholesterol with diet, exercise, and in some cases, cholesterol-lowering medication. This can help prevent xanthelasma from coming back—and improve your overall health. Here are some ways to lower your cholesterol: